Mbeya, Tanzania 2019

Rob Razick, MD
Dr. Razick is a graduate of the Medical University of South Carolina and member of the Prisma Health Midlands EM class of 2020. He is pursuing a Global EM Fellowship at University of Kentucky after completion of his residency.
.jpeg)
As I got off the plane in Mbeya, Tanzania I was greeted with a “Mambo”, a friendly smile, and a thermometer to the forehead. I knew any reading greater than 38 degrees centigrade would greatly alter my time in Africa. Images of “The Bubble Boy” immediately came to mind. “Click”. A reading of 36. degrees was my ticket into the country. I hadn’t been so relieved to just be “normal” since junior high gym class.
Dr. Prosper Bashaka, our gracious host, was waiting for us at the airport to take us to our home for the next 2 weeks. Mbeya is a city located in southwest Tanzania. It is nestled at the base of Loleza peak at an altitude of about 5,500 feet (and you can feel every single foot of elevation). Although the city itself has only a population of around 300,000, the Mbeya region population totals around 2 million people.
My initial posse was comprised of myself, a co-resident, a 4th year medical student, and a neighborhood-friendly ER nurse. Not to mention our housemates - a family of South African
missionaries, German linguist, and what seemed like a Noah’s Ark contingent of farm animals in the yard. The roosters were sure not to let us oversleep, or sleep at all really. Reinforcements in the form of our ED global health fellow, fellowship director, and multiple other attending physicians would join us in one weeks’ time.
Over the first week of our trip, we spent time in the Emergency Department at Mbeya Zonal Referral hospital. We met many of the general practitioners and nurses of the ED. One of our first patients was a middle aged man agitated from being accidentally engulfed in sand. He required multiple doses of IM ketamine and lorazepam for sedation as he was “mooing”. I’ve never been so far away from home and at the same time felt so close. A negative head CT would follow in the next several days. We also spent time in the ICU learning how the most critically ill patients were cared for at the hospital.
As we all came to discover, dealing with common emergencies in a resource limited environment turned out to be quite the challenge. Auscultating a patient’s lungs with a chief complaint of
dyspnea takes on a whole new significance when a chest x-ray cannot be readily obtained. Taking care of a child involved in a motorcycle crash with signs of traumatic brain injury without being able to obtain a STAT Head CT was such a foreign concept to me. Throughout my time in the hospital, I gained a whole different kind of respect for the healthcare workers trying their best in this resource limited environment. Trusting your hands, eyes, stethoscope, and the occasional bedside ultrasound is of the utmost importance. It will definitely make me think twice before I complain about a chest x-ray taking an hour instead of 30 minutes back home.
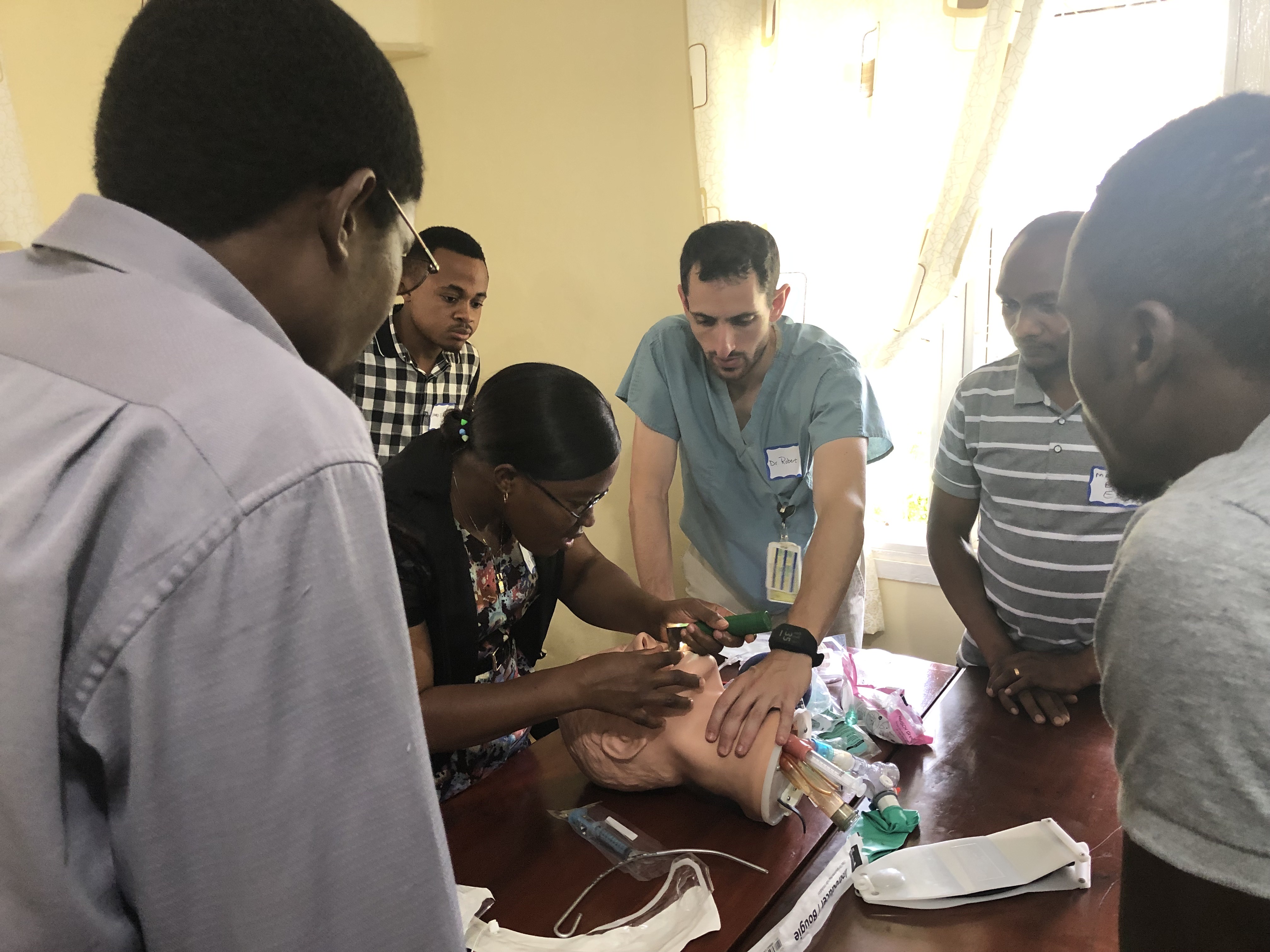
After our full team arrived, the second week of our time in Mbeya was mostly spent in the classroom. Monday and Tuesday were spent giving critical care training to the ED/ICU staff. We gave lectures on respiratory failure and management, ventilator settings, and multiple other critical care topics. We also led small group hands-on learning sessions with simulation mannequins and simulation cases. These sessions allowed the nurses and physicians to practice some of the fundamental concepts we had tried to reinforce over the previous days.

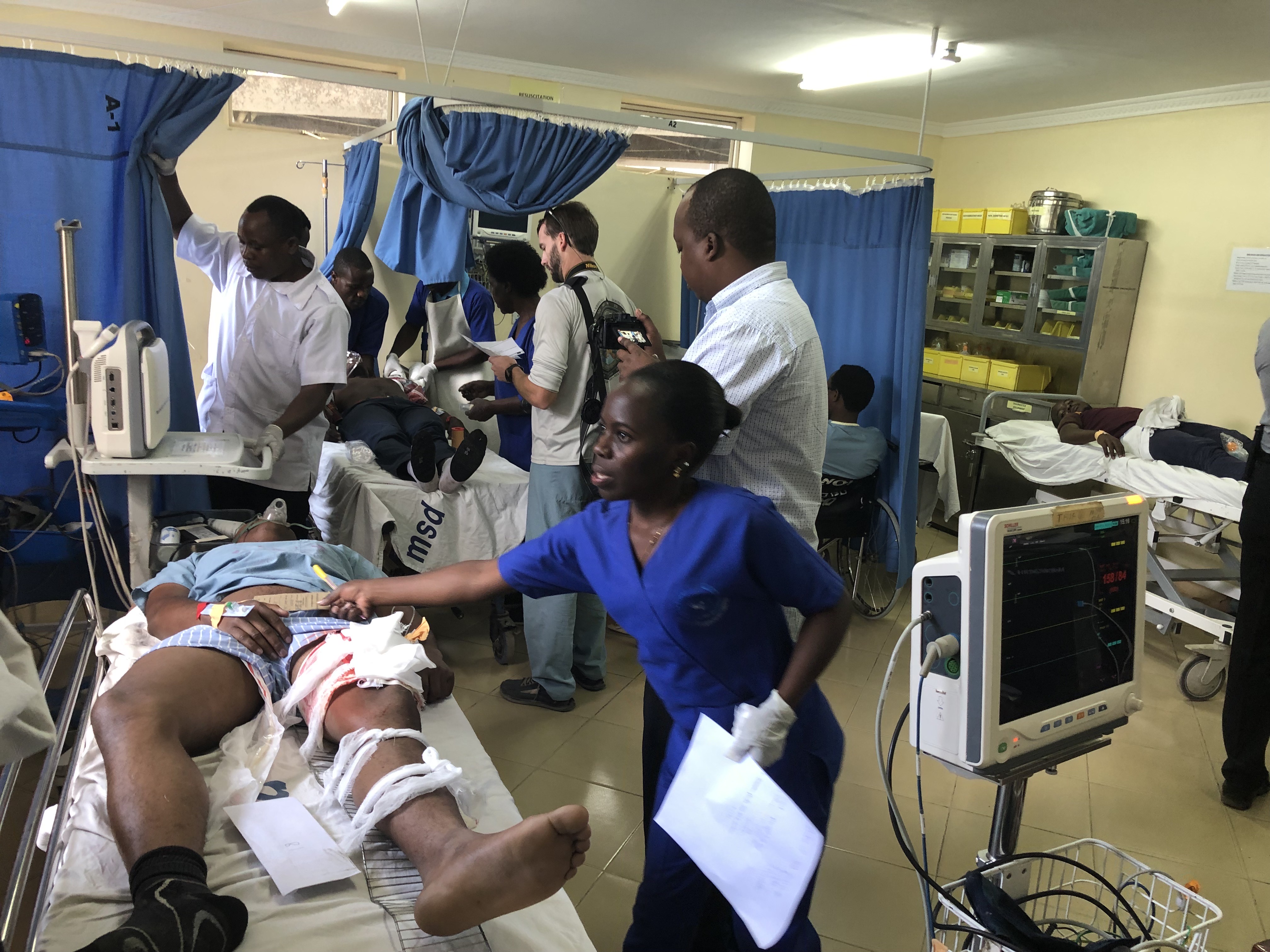
Wednesday and Thursday were focused on disaster drill training. A lecture discussing the appropriate triage and management of a mass casualty event was given. The following day, a mass casualty practice drill was set up with medical students from the local medical school volunteering as patients involved in a bus crash. No Emmys were handed out for the acting, but I definitely could have been fooled into dealing out more than a few yellow cards. The effort was second to none. The ED staff rose to the occasion and seemed to really grasp many of the concepts taught to them the day prior.
All in all, our time in Africa was a great experience. I fully anticipate repeat trips in the future. We all hope to continue the collegial relationships we have formed with so many of the doctors and nurses in Mbeya. Also, we’re all crossing our fingers hoping that we don’t have to learn about any tropical diseases, like malaria and schistosomiasis, first hand as we travel back to the U.S. But either way, I’d still say the swim in Lake Malawi was totally worth it.













 Back to Locations List
Back to Locations List